Article Topic: The relationship between nutrition and multiple sclerosis
Author: Raghad AL-derawi
Editor: Alaa Abu- Shaweesh
Reviewer: Ethar Hazaimeh
Keywords: Multiple sclerosis, obesity, Westernized diet, vitamin D, active compounds of curcumin.
Abbreviation: Multiple sclerosis ( MS ), body mass index ( BMI ), western diet ( WD ), central nervous system ( CNS ), saturated fatty acids (SFA), omega-6 polyunsaturated fatty acids (PUFAs), reactive oxygen species (ROS).
Abstract
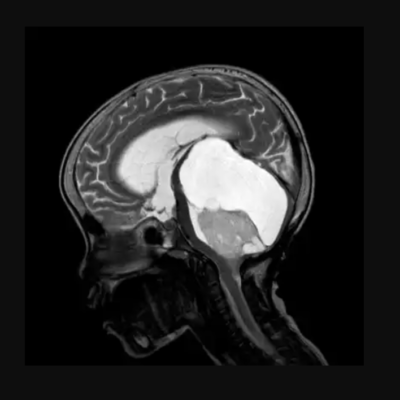
Multiple sclerosis (MS), a neurodegenerative illness affecting the central nervous system, stems from an autoimmune response and is characterized by inflammatory demyelination and axonal transection (17). This study investigates the impact of various factors including the Western diet, obesity, microbiota composition, and levels of vitamin D, curcumin, and melatonin on MS. Our findings suggest that the consumption of saturated fats and sugar-rich foods may escalate immune system activity, potentially exacerbating MS. Additionally, individuals with a high body mass index (BMI) face a doubled risk of developing MS. Moreover, curcumin shows promise in alleviating MS symptoms. While previous research indicates that low levels of melatonin and vitamin D may predispose individuals to MS, further studies are needed to elucidate their individual effects on the condition.
Introduction
Multiple sclerosis (MS) afflicts over 2.5 million individuals worldwide, constituting a chronic inflammatory and demyelinating disorder of the central nervous system (CNS) (1). Typically emerging in adulthood, MS primarily strikes individuals aged 20 to 40, with a notable 3:1 female-to-male ratio (2).
At the crux of MS lies its defining feature: localized lymphocytic infiltration within the CNS, precipitating myelin degradation and axonal damage. This cascade culminates in a spectrum of neurological symptoms and physical debilitation. Notably, the location of CNS lesions significantly influences the clinical presentation of MS. Affected individuals often contend with fatigue, pain, spasticity, compromised motor function and coordination, sensory disturbances, visual impairments, and cognitive deficits (1).
Additionally, approximately 85–90% of individuals grappling with MS contend with its relapsing-remitting form, characterized by episodic exacerbations of symptoms followed by periods of remission. Moreover, nearly half of MS patients experience a secondary progressive phase, wherein symptom recovery is incomplete and the disease progressively worsens. A defining trait of progressive MS is the inexorable accrual of neurological impairment over time (1).
Notably, a multitude of studies have underscored the multifaceted influences shaping multiple sclerosis, with nutrition emerging as a significant factor. Given that nutritional elements may exert their effects even before the onset of MS symptoms, discerning the precise dietary pathways contributing to the disease poses a formidable challenge (4). However, empirical evidence suggests a correlation between high prevalence rates of MS and regions renowned for their consumption of hypercaloric, high-fat, high-carbohydrate “Western” diets, replete with processed foods and saturated fats.
Despite numerous investigations linking diet to MS, the efficacy of nutritional interventions as adjunctive care remains contentious. Recent research reveals that a substantial portion of MS patients fail to meet recommended dietary intake levels of fruits, vegetables, and whole grains. Early observations by Swank et al. in the 1950s indicated a diminished incidence of MS in individuals consuming lower amounts of animal fat. Studies employing animal models of MS have demonstrated that the effects of saturated fats vary depending on their aliphatic chain length, yielding both deleterious and beneficial outcomes (4).
Moreover, the presence of natural antioxidants in food plays a pivotal role in human health. Whether enzymatic or non-enzymatic, these compounds serve as formidable defenders against free radicals, safeguarding the body from oxidative stress. Previous studies have unveiled a significant correlation between diminished levels of antioxidant vitamins and melatonin in MS patients compared to controls.
Notably, glutathione, a critical antioxidant in the brain, is depleted in individuals afflicted with MS. Nonetheless, the precise temporal dynamics, extent, and underlying mechanisms through which antioxidants exert their influence on multiple sclerosis necessitate further elucidation. Food constituents can directly modulate various cellular components, shape gut microbiota composition, and influence immunological and metabolic processes (4).
In this study, our objective is to systematically evaluate the studies concerning the influence of diet and lifestyle on MS.
The effect of obesity on MS
Obesity is one of the environmental factors influencing the development of MS (16). To assess obesity levels, researchers utilized (BMI) and waist circumference measurements. A BMI falling between 25 and 29.9 kg/m² indicates overweight, while 30 kg/m² or higher indicates obesity. Abdominal adiposity was also considered, with thresholds set at 102 cm for men and 88 cm for women (16). A 2019 study suggested that individuals with a BMI of 27 kg/m² or higher during adolescence and childhood may face double the risk of developing MS (16). Despite significant strides in understanding the pathophysiological connections between obesity and MS, further research is necessary to fully comprehend the impact of obesity on MS (16).
The transition to a Westernized diet carries significant implications for MS
Western diet (WD): The Western diet is characterized by its reliance on processed foods, fast food, convenience products, snacks, and sugary soft drinks, often deficient in essential fibers, vitamins, and minerals (7). Prolonged adherence to a Western diet may disrupt physiological balance and health by fostering weight gain, adverse alterations in lipid and energy metabolism, and triggering immune system activation (7).Where recent research, conducted in 2018, uncovered a notable association between higher BMI and increased vulnerability to MS across various age groups, encompassing both children and adults (8). Additionally, an elevated intake of specific fats, notably saturated fatty acids (SFA), omega-6 polyunsaturated fatty acids (PUFAs), and trans-fatty acids, alongside a concurrent decrease in omega-3 PUFA consumption, has emerged as a contributing factor to the rising incidence of MS (8).
MS and active compounds of curcumin
In the realm of alternative therapies for managing the symptoms of MS, curcumin stands out as a promising candidate. Derived from turmeric, curcumin has been studied for its purported ability to alleviate MS symptoms. In this article, we delve into the properties and potential benefits of curcumin in mitigating the effects of MS. Curcumin, also known as diferuloylmethane, is the active compound found in turmeric, originating from the rhizome of the East Indian plant Curcuma longa. Comprising curcuminoids, commercially available curcumin consists primarily of curcumin (77%), demethoxycurcumin (17%), and bisdemethoxycurcumin (3%). Notably esteemed for its antioxidant capabilities, curcumin plays a crucial role in directly neutralizing toxins generated from reactive oxygen species (ROS). This attribute equips curcumin with the potential to positively influence multiple sclerosis by counteracting ROS accumulation stemming from transition metal build-up in the brain. Furthermore, curcumin demonstrates efficacy in preventing protein aggregation within the brain, thereby offering potential benefits in mitigating the onset of neurodegenerative disorders (9).
The relationship between melatonin and MS
Melatonin, a neurohormone primarily synthesized in the pineal gland by the circadian rhythm, exhibits pleiotropic effects. Beyond its role in regulating the sleep-wake cycle, melatonin possesses antinociceptive, antidepressant, anxiolytic, and immunomodulatory properties (10). Studies have yielded mixed findings regarding melatonin levels in MS patients, with some indicating decreased levels compared to controls, while others find no significant difference (10). Although several studies suggest that low melatonin levels may pose a risk factor for MS, further research is warranted to elucidate the precise impact of melatonin on the disease (11).
The influence of vitamin D on MS
Various factors, including inadequate sun exposure, metabolic dysfunction, and limited bioavailability, can impact vitamin D levels. Diminished exposure to sunlight, the primary source of vitamin D, has been associated with an increased risk of developing multiple sclerosis (MS), as well as exacerbations of the disease and a heightened likelihood of relapses (6). Indeed, insufficient sun exposure and reduced availability of vitamin D are often correlated with the geographical distribution of MS. Studies have shown significantly lower serum concentrations of vitamin D in MS patients compared to healthy individuals, suggesting a potential link between vitamin D deficiency and the risk of MS.
Microbiota and MS
Some studies have shown no discernible difference in the composition of microbiota between individuals with MS and those without the condition (12). However, a study conducted in 2023 identified alterations in the microbiota of MS patients, particularly in the production of short-chain fatty acids (13). Further research is necessary to elucidate the precise alterations in microbiota among individuals with MS and to understand how dietary interventions can potentially modulate these alterations.
Conclusion
Current epidemiological studies have robustly demonstrated a correlation between dietary factors and MS. Specifically, research has underscored the potential influence of several components including vitamin D, curcumin, melatonin, the Western diet, microbiota composition, and obesity on the development and progression of MS. While these findings offer valuable insights into the multifaceted nature of MS etiology, further comprehensive investigations are imperative to elucidate the precise mechanisms and interplay of these factors in the context of MS pathogenesis. Enhancing our understanding of these relationships holds significant promise for informing targeted interventions and therapeutic strategies aimed at mitigating the burden of MS.