Article topic: Management of Acute Ischemic Stroke
Author: Zain Alsaddi
Editor: Ethar Hazaimeh
Keywords: Acute ischemic stroke, Revascularization, rTPA, IV thrombolysis, Endovascular Therapy.
OVERVIEW
A multidisciplinary approach that involves the critical care of specialists has been established to treat an acute ischemic stroke (AIS) attack. Before the 1990s, treatment options for AIS were limited and they mainly focused on managing the patient’s symptoms, secondary prevention as well as rehabilitation. 2
However, since then, two major innovations were introduced into the field that lead to a dramatic transformation of the care of an acute stroke attack. In 1995, the use of IV tissue plasminogen (IV-tPA) was approved by the Federal Drug Administration (FDA) based on a landmark study conducted by the National Institutes of Neurological Disease and Stroke (NINDS). 3
For almost 2 decades, IV-tPA remained the mainstay of treatment. In 2015, more sophisticated clinical trials were conducted and showed robust outcomes for the use of endovascular therapy (EVT). 4
Early detection
Stroke is a clinical diagnosis; therefore, the first key step is the early identification of an acute stroke attack. As it may occur in a hospital setting or anywhere else in the community, it is important that bystanders are able to recognize it and act as fast as possible in order to deliver the appropriate treatment for the patient.
Starting with the prehospital setting, the BEFAST acronym is the algorithm that was made popular by the American Heart Association/American Stroke Association to diagnose stroke easily. To achieve a diagnosis, all these symptoms must be present.
The BEFAST acronym stands for:
- Balance: sudden onset of losing of balance or coordination
- Eyes: blurry or unclear vision, double vision
- Facial droopiness, weakness, or asymmetry
- Arm and/or weakness
- Speech difficulty or slurring
- Time of onset of the symptoms.
Another way to identify signs of an acute stroke attack is the presence of the 6S:1
- Sudden onset of symptoms
- Slurred Speech (The patients’ words become unclear and hard to understand.)
- Side Weak (weakness is seen on one side of the body like the face, arm, or leg or all three can get weak)
- Spinning (vertigo)
- Severe headache
- Seconds (take note of the time the patient was last seen normal and the time the symptoms appeared)
Early recognition activates a stroke-specific chain of survival known as the 8Ds of stroke care chain:2
- Detection: involves recognition of the signs and symptoms of an acute stroke attack.
- Dispatch: usually includes calling 911 to activate Emergency medical services.
- Delivery: refers to prompt delivery of the patient to the hospital for further evaluation by specialists.
- Door: refers to the patient’s arrival at the emergency department. The patient must be assessed with 10 minutes of arrival by an ED physician, according to the recommendations from the National Institute of Neurological Disorders and stroke.
- Data collection includes both physical and neurological exams as well as laboratory tests.
- Decision of the appropriate treatment method is made once the data has been assessed.
- Drug/device: involves the administration of fibrinolytic therapy with 4.5 hours of the onset of symptoms.
- Disposition: it is recommended to admit the patient to the ICU or stroke unit within 3 hours of his arrival.
It is recommended to use the NIH stroke scale to completely assess a patient presenting with stroke symptoms. The patient should be examined by a trained physician or a neurologist within 10 minutes of arrival to the emergency room.
PRINCIPLES OF ACUTE STROKE CARE
There are three main principles of acute stroke:
(1) Achieve timely recanalization of the occluded artery and reperfusion of the ischemic tissue
(2) Optimize collateral flow
(3) Avoid secondary brain injury.
The mainstays of acute stroke treatment are recanalization and reperfusion, which can reduce the size of the infarct and reverse neurologic deficits. Recanalization is defined by the degree at which an occluded artery can be reopened. Without recanalization, the ischemic penumbra is surely destined to progress to infarction. Reperfusion is measured by the degree of flow reaching the previously hypo-perfused brain region.
Collateral flow is responsible for maintaining the viability of the ischemic penumbra. It provides enough flow to prevent critical ischemia and infarction, but the flow isn’t sufficient to maintain normal cellular function. it can be protected by monitoring and avoiding blood pressure drops and is also supported by IV fluids administration.
In the emergency department. The initial evaluation of a patient with a possible acute stroke presentation mainly focuses on establishing whether the patient is eligible for reperfusion therapy. Necessary information is collected about the patient. This includes the time the patient was last seen or known to be well, his medical condition, and any recent surgery that could contraindicate thrombolysis. A neurologic examination is performed in order to calculate the National Institutes of Health Stroke Scale (NIHSS) score, a capillary glucose level, blood pressure as well as brain imaging are done.
Revascularization
The main and primary goal of managing advanced stroke is revascularization and limiting the possibility of a secondary neuronal injury. For selected patients, IV thrombolysis and EVT are now available.
IV thrombolysis
In 1995, the transition in the treatment for AIS from being purely and completely symptomatic to a highly time-sensitive matter was proven in the first landmark clinical trial which proved the use of IV-tPA to be safe and efficient. It shows that, on the 90-day mark, if IV-tPA is administered within the first 3 hours of symptoms onset, patients are at least 30% more likely to have only minimal or no disability.
in 2009, the American Heart Association/American Stroke Association (AHA/ASA) extended the IV-tPA window from 3 to 4.5 hours. Based on the European study Thrombolysis with Alteplase 3 to 4.5 Hours after Acute Ischemic Stroke (ECASS-3). This extension led to an increase in the utilization of IV-tPA by up to 20%. 5,6,7
In recent clinical trials, it was suggested that imaging rather than the known time of onset, which is the last time the patient was seen normal, can guide clinicians to treat patients using the time discrepancies of acute stroke showing. Data obtained from a clinical trial conducted by the European multicenter, MRI-Guided Thrombolysis for Stroke with Unknown Time of Onset (WAKE-UP) suggested that almost 50% of wake-up strokes and strokes that occur during the daytime and have an unknown onset are IV-tPA candidates when MRI criteria are used. However, due to its cost, time spent in metal screening as well as the often far distance to the scanner, its implementation is limited. In another clinical trial where Thrombolysis- Guided-by Perfusion Imaging was performed up to 9 Hours after Onset of Stroke (EXTEND). CT-P imaging was used to assess the eligibility for IV-tPA and suggested that the efficacy and safety of IV-tPA can extend up to 9 hours and that revascularization can extend up to 24 hours. 8,9
The US Food and Drug Administration (FDA) has only approved rtPA for use within 3 hours of stroke onset, but regulatory agencies in most other countries, those in the European Union are included, have approved its administration within 4.5 hours of stroke onset. However, according to the American Heart Association (AHA)/American Stroke Association, 4.5 hours is the recommended time window.18
The narrow therapeutic window and the fact that it is less effective in cases of large-vessel occlusions (internal carotid, initial segment of the medial cerebral artery, basilar artery) or large thrombi are considered as a limitation of this treatment. 15,17
The indications and contraindications for IV rtPA have been revisited in the most recent version of the AHA guideline for the management of acute stroke and modified by the FDA in the package insert for the drug. 14, 18
| American Heart Association Guideline 2019 | US Food and Drug Administration (FDA) Package Insert 2015 |
| Indications | |
| Diagnosis of ischemic stroke with disabling neurologic deficit (regardless of severity) | Same |
| Symptom onset within 4.5 hours | Within 3 hours |
| Wake-up stroke with a diffusion-weighted imaging-FLAIR mismatch on MRI | Not mentioned |
| Age ≥18 years | Warning for age >77 years with risk factors for intracranial hemorrhage |
| Contraindications | |
| Severe head trauma within 3 months | Contraindicated |
| Ischemic stroke within 3 months | Removed |
| Previous intracranial hemorrhage | Warning for recent intracranial hemorrhage (contraindicated if active intracranial hemorrhage) |
| Suspected subarachnoid hemorrhage | Contraindicated |
| Suspected infective endocarditis | Not listed |
| Suspected aortic arch dissection | Not listed |
| Recent intracranial or intra-spinal surgery (within 3 months) | Contraindicated |
| Intracranial intra-axial neoplasm | Not listed |
| Gastrointestinal malignancy or gastrointestinal bleeding
within previous 21 days |
Warning |
| Active internal bleeding | contraindicated |
| Systolic blood pressure >185 mmHg or diastolic blood pressure >110 mmHg that cannot be lowered safely | Contraindicated for severe uncontrolled hypertension. Warning for BP >175/110 mmHg. |
| Bleeding diathesis
International normalized ratio (INR) >1.7 Heparin within 48 hours with abnormal activated partial thromboplastin time (aPTT). Low-molecular-weight heparin full treatment dose within the previous 24 hours. Platelets <100,000/ mm3 Current use of direct thrombin inhibitor or factor Xa inhibitor with abnormal coagulation tests. |
Contraindicated for bleeding diathesis |
| CT showing acute hemorrhage | contraindicated |
| CT showing extensive hypo-density (eg, >1/3 of the cerebral hemisphere) | Removed |
Table 1
By far, the most effective treatment for acute ischemic stroke is Acute reperfusion. The treatment of acute stroke also includes adequate management of the hemodynamic state of the patient, monitoring and managing ischemic brain edema, as well as early recognition of and therapy for systemic complications such as infections, cardiac arrhythmias, heart failure, and venous thromboembolism in a stroke unit staffed by specially trained personnel.
IV thrombolysis’ wide adoption that began 25 years ago has recently been followed with clear evidence that adding endovascular treatment along with mechanical thrombectomy to the treatment of acute stroke onset can further improve the outcomes in patients with severe neurologic deficits from a proximal intracranial vessel occlusion.
The standard dose of IV rtPA administered for acute ischemic stroke is 0.9 mg/kg, with 10% of the dose is administered as a bolus while the remainder is infused over 1 hour. The total dose should not exceed 90 mg. the drip-and-ship strategy is followed in the emergency departments of medical centers that have more limited capabilities, where the patients first receive the bolus of rtPA and then get transferred to a primary or a comprehensive stroke center while the rest of the dose of the drug gets infused.
In ischemic stroke, no other thrombolytic agent has been approved for use. however, there is growing information on the value and efficacy of Tenecteplase when used for treating patients with acute cerebral ischemia. Tenecteplase is a bioengineered variant of rtPA that has a longer half-life, greater fibrin specificity as well as increased resistance against tissue plasminogen inhibitor-1 compared to rtPA. Therefore, it is administered as a single IV bolus.
A clinical trial is known as The NOR-TEST (Norwegian Tenecteplase Stroke Trial) was conducted to test the safety and efficacy of Tenecteplase 0.4mg/kg (up to 40mg) versus the standard dose of rtPA within 4.5 hours of the onset of an acute ischemic stroke. The proportions of patients with serious adverse events, including symptomatic intracerebral hemorrhage (ICH), and functional independence at 3 months were similar in the Tenecteplase and rtPA groups. However, the authors could not conclude that the two treatments were equivalent because the trial had been designed to test only for superiority. 19
Another clinical trial was conducted which assigned patients with acute ischemic stroke and a proximal intracranial artery occlusion eligible for mechanical thrombectomy randomly to receive Tenecteplase (0.25 mg/kg, up to 25 mg) or standard-dose rtPA within 4.5 hours of symptom onset. In this trial, known as The EXTEND-IA TNK (Tenecteplase Versus Alteplase Before Endovascular Therapy for Ischemic Stroke) trial, the Patients who received treatment with Tenecteplase had higher rates of recanalization/reperfusion at the time of initial assessment by conventional angiography, 22%versus 10%with rtPA. At 3 months, they also had a better functional outcome with similarly low rates of symptomatic ICH (1% in both groups). Thus, if future studies confirm such promising results, Tenecteplase may become a preferred alternative to rtPA. 20
Endovascular Therapy
Since 1996, the only standard care trusted for acute ischemia has been Intravenous tissue plasminogen activator (IV tPA) however, this treatment has been used in only a small portion of acute ischemic stroke patients due to many contraindications and the low rates of recanalization/reperfusion in large vessel occlusions.
Although the FDA approved the use of IV-tPA, up to 69% of stroke patients are ineligible to receive IV-tPA due to delayed hospital presentation. Thanks to Endovascular treatment (EVT) the time window for AIS treatment has expanded providing the physicians with a stronger therapeutic arsenal over the last 3 years. The interventions for stroke with Endovascular therapy offer theoretical advantages over intravenous fibrinolysis, which include speed and rate of recanalization, reduced risk of hemorrhage, and a longer time window for use. 22
Substantial efforts have been made in order to explore other possible treatment modalities that could improve clinical outcomes, particularly endovascular therapy (EVT) using mechanical devices. The EVT devices, which were approved by the Food and Drug Administration (FDA) in the United States for the treatment of acute ischemic stroke in 2004, 2008, and 2012 were the Mechanical Embolus Removal in Cerebral Ischemia (MERCI) Retriever, the second-generation of mechanical device the Penumbra System and the third-generation stent retrievers, respectively. 23
The degree or quality of revascularization indicates the success of EVT. The Thrombolysis in Cerebral Infarction scale, shown below, is a tool used to standardize the different degrees of reperfusion ranging from no perfusion (TICI 0) to complete perfusion (TICI 3). TICI scores of 2B to 3 are usually regarded as successful reperfusion. 10,11,12
| Grade | Radiographic Features |
| 0 | No perfusion beyond the point of occlusion. |
| 1 | Penetration with minimal perfusion. Contrast passes the obstruction but fails to visualize the entire cerebral bed beyond the point of obstruction. |
| 2 | Partial perfusion. Contrast passes the obstruction and visualizes the cerebral bed past the obstruction. However, the flow of contrast in the distal bed is slower than in other non-obstructed vessels. |
| 2A | Only <2/3 of the entire vascular territory is visualized. |
| 2B | Complete visualization of the vascular territory but with slower filling than normal. |
| 3 | Complete perfusion. The entire vascular territory is visualized with normal flow. |
Table 2: Thrombolysis in Cerebral infarction scale. (TCIS)
Candidates for Acute Endovascular Stroke Therapy:
◆ Age ≥18 years
◆ National Institutes of Health Stroke Scale score ≥6
◆ Time from symptom onset to groin puncture <6 hours (up to 24 hours if evidence of sizable ischemic penumbra is seen on perfusion imaging)
◆ Good pre-stroke functional status
◆ Alberta Stroke Program Early CT Score ≥6 on baseline CT scan
◆ Presence of proximal intracranial artery occlusion
During endovascular therapy, the patient is usually put under General anesthesia (GA) and conscious sedation which allows a completely motionless procedure. This may however be associated with significant disadvantages including hemodynamic fluctuations in cerebral perfusion pressures and time delays. standardly, the common femoral artery is used as an access route for percutaneous neuro-interventions but in some patient subsets, including those with severe systemic atherosclerosis with bilateral iliofemoral artery occlusions, thoracic aortic dissection, extreme tortuosity, ostial stenosis of the proximal cervical vasculature, or unfavorable anatomy of the aortic arch pose a challenge during the procedure.21
The best imaging modality to select patients for acute endovascular intervention is yet to be determined. Evaluation of early ischemic changes on a non-contrast CT is indispensable, but the relative value of collateral flow assessment by non-invasive angiography and degree of perfusion deficit by CT or MRI perfusion scans continues to be debated for patients presenting within the first 6 hours after symptom onset.
Below is a diagram that illustrates the steps followed when handling a patient presenting with an acute ischemic stroke event. 24
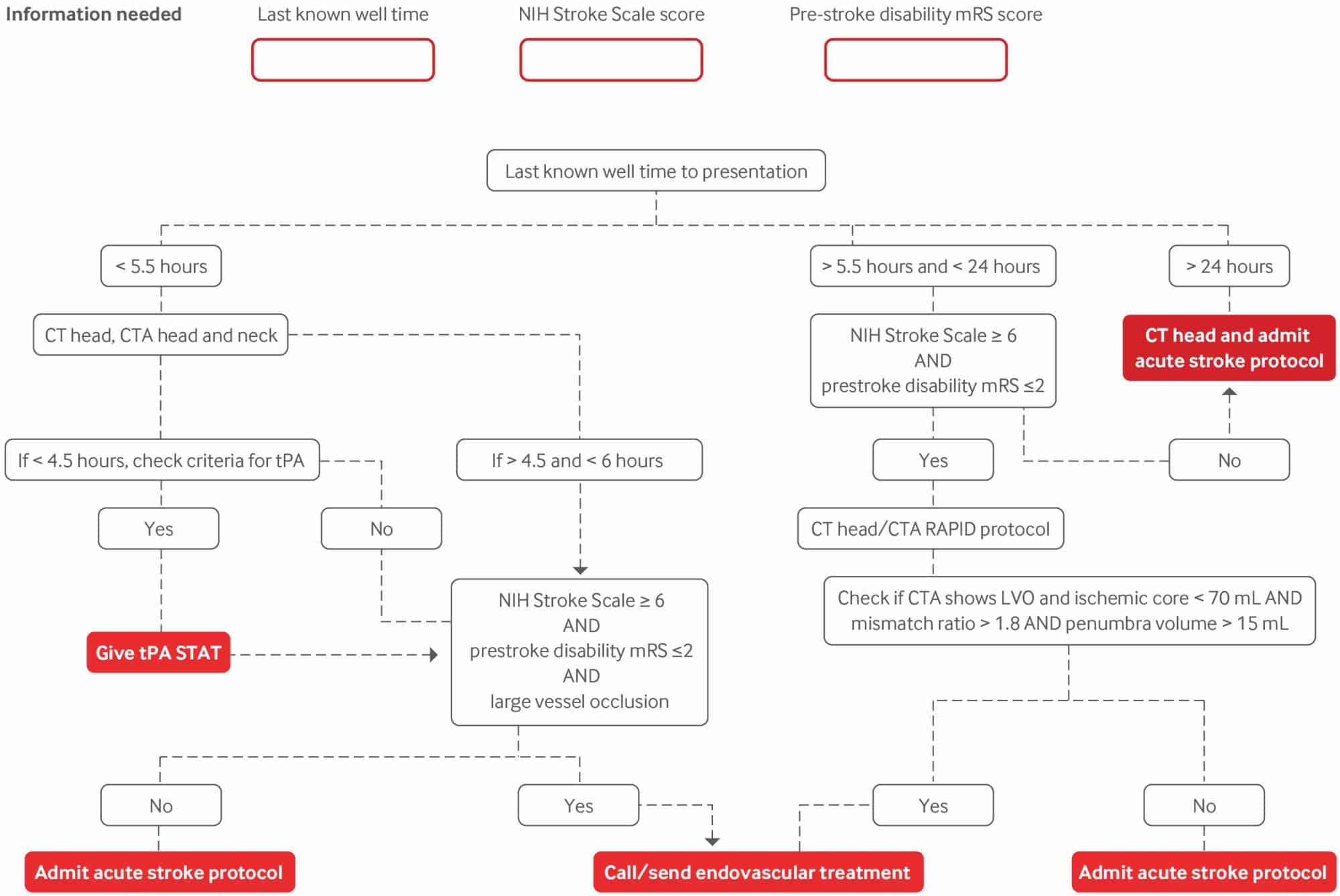
Acute Ischemic Stroke Protocol 24
CONCLUSION
Acute ischemic stroke is a medical emergency in which every minute counts. The main target is to achieve reperfusion and reverse neurologic deficits to allow patients to regain function, even in severe cases. Two reperfusion strategies are now proven: IV rtPA and mechanical thrombectomy. for the right candidates, they are both safe and effective. Patient selection is crucial to optimize outcomes, but the attitude of the clinician should be that treatment should be given unless a solid contraindication exists. Efforts continue to expand indications for endovascular therapy, both within the early and extended time windows and those efforts should also be concentrated on refining systems of care to allow more patients to have access to reperfusion treatment.