Topic: Binge Eating disorder (BED)
Author: Sohail Batarseh
Editor: Ihdaa Bani Khalaf, Sadeen Eid
Reviewer: Ethar Hazaimeh
Keywords: Binge eating disorder, Obesity, Eating dysregulation, Treatment, COVID-19.
Introduction
Eating disorders are fatal and incapacitating mental illnesses that severely damage physical health and interfere with psychosocial functioning.1 Moreover, attitudes toward food, weight, and body image significantly influence the development and maintenance of eating disorders such as Binge eating disorders.1
Binge Eating disorder (BED) was first listed in the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV), as an eating disorder provisional diagnosis under the heading of Eating Disorder Not Otherwise Specified.1 It is now classified as a stand-alone diagnosis in the proposed Draft Revisions Disorders and Criteria for DSM-52 (Diagnostic and Statistical Manual).
Diagnostic systems recognized the basic feeding and eating disorders and it covered six primary food and eating disorders: Anorexia nervosa, bulimia nervosa, binge eating disorder, avoidant-restrictive food intake disorder, pica, and rumination disorder 3.
Binge eating disorder BED is characterized by recurrent binge eating episodes in the absence of proper compensatory behavior such as fasting, purging, or strenuous activity.3 It is closely related to obesity because it involves calorie overconsumption .4 BED is far worse than overeating since it is linked to more tremendous subjective suffering over eating behavior, it commonly lowers the quality of life and is connected to psycho-pathological traits mainly stress, negative effects, depression, or anxiety, and can be comorbid with diseases such as metabolic syndrome, which mostly includes type 2 diabetes, hyperparathyroidism, and hypertension.5 There is still much to learn about the etiology of BED, besides there are a lot of categories of risk factors for eating disorders: social, psychological, biological (including genetic and more). 2
Epidemiology and Etiology
A study on the risk factors for the emergence of ED points to the significant importance of biological components. Although neither gene nor genome-wide research has discovered really verified genes for eating disorders, the role of genetic variables on the emergence of an ED is suggested.6
Data on the prevalence of Bulimia Nervosa and Binge Eating differ depending on the country, in the US a survey estimated the prevalence to be 0.6% for AN (Anorexia nervosa), 1.0% for BN, and 2.8% for BED.7 When we look at AN(Anorexia nervosa) and BN, which occur in a 1:9 male-to-female ratio, we notice the male-to-female ratio is more balanced in BED about 4:6.8 The interaction of biological variations between men and women and the unequal impact of sociocultural variables on the sexes have been hypothesized to be the cause of the sex differences in EDs (eating disorders).4
Among other biological variations, scientists believe that estrogen’s organizational effects during puberty encourage the formation of BEDs in genetically susceptible females.9 Recent research investigated differences between 208 men and 1117 women using data from 11 randomized controlled psycho-social BED therapy treatments these studies used Baseline and outcome symptoms to assess via the interview and questionnaire versions of the Eating Disorder Examination (EDE), women and men reported similar levels of dietary restraint and binge-eating episode frequencies at baseline .5
In comparison to women, males expressed much fewer worries about their physical appearance, weight, and eating habits. Men and women did not substantially differ after treatment in terms of the: overall EDE score, the number of binge-eating events in the previous 28 days, the remission of binge eating, or early study dropout.10
Although the frequency of eating disorders has grown by 25% worldwide, only around 20% of those patients seek treatment.11
Psychopathological features associated with BED
FA (food addiction) refers to compulsive overeating that resembles addiction and is marked by cravings and difficulty avoiding high-calorie meals.12
Although FA (food addiction) could seem to be comparable to BED (binge eating disorder), it’s crucial to remember that FA (food addiction) is still a contentious notion that hasn’t yet been acknowledged as a diagnostic entity, whereas BED is a recognized and diagnosable mental condition.6
Between 30.0 and 80.0% of people with BED have comorbid mood and anxiety problems at any given moment13and sometimes there are certain associated diseases like bipolar illness14 The majority of BED patients also have impairments in their psychological health, which might include issues with autonomy, environmental mastery, and self-acceptance15 and overvaluation of body shape and weight, which is closely linked to mental distress, eating-related psychopathology, and an even worse prognosis for the disease.16
Neurobiology
The exposure to enticing food signals affected several groups, including obese and non-obese people as well as those with bulimia nervosa, by an increase in activity in the insula and the orbitofrontal cortex (OFC).17 Not surprisingly, these areas of the brain correspond to the major and secondary taste cortices. In recent research, while perceiving appetizing food signals, people with BED in particular exhibit higher prefrontal activity in comparison to other disordered eating groups and healthy control participants.18
These early results lend to the theory that BED patients are more sensitive to food rewards. Additionally, using a classification analysis based on neural responses as people view appetizing foods shows that activity in many reward processing regions, including the orbitofrontal cortex (OFC) and striatum, identifies people with BED in comparison to non-BED obese or BN(bulimia nervosa) people with a fair degree of accuracy. 19
In the last 100 years, researchers made the first discoveries of how the ovarian cycle affects food intake in intact female rats and how the removal of the ovaries causes an accumulation of fat tissue in the previous century, the menstrual cycle has been linked to fluctuations in women’s appetite and satiety.20
Ovarian hormones operate as gene transcription factors in several neurobiological systems that are known to be connected to disordered eating behavior, suggesting that they may have a genetic impact on the central nervous system.21
Even though the majority of research on BED neurobiology has been conducted in females, the effects of ovarian hormones on eating behavior and weight management have not been scientifically shown.7
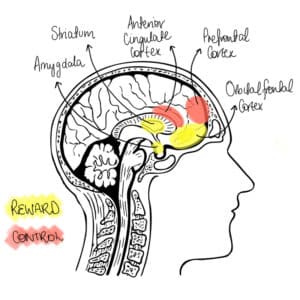
Figure 1. this figure represents increased activity in the emotional center of the brain – the amygdala and increased activation of the reward network striatum and orbital frontal cortex fails to, self-control and planning network frontal cortex and anterior cingulate cortex remain underactive. 22
Treatment
There is a lot of pharmaceuticals, physiological and recent advanced treatment. Findings show that BED diagnosis is clinically useful in producing unique results across various therapy.2
Psychological Treatment
Cognitive-behavioral therapy
Cognitive behavioral therapy (CBT) is a type of psychological care that is useful for a variety of issues, such as depression, anxiety disorders, …. etc.8
More than 50% of patients who get Cognitive-behavioral therapy have complete recovery from binge eating, as well as significant improvements in the related depression, psychosocial functioning, and particular eating disorder psychopathologies such as overvaluing body form and weight.9
IPT (Interpersonal Psychotherapy)
Has been modified for the treatment of both bulimia nervosa and BED. IPT(interpersonal Psychotherapy) was initially created as a brief, manual-based psychotherapy for depression.9 The focus is mostly on assisting patients in identifying and resolving interpersonal issues that are currently plaguing them and supporting their eating disorders. The therapy is noninterpretive and non-directive.9
Guided self-help
Self-help therapies based on CBT principles are the subject of an expanding corpus of research. A self-help book plus a small number of brief therapy sessions delivered by medical professionals with varied levels of CBT experience and skill make up guided self-help (CBTgsh).9
Pharmacologic Therapy
Research has focused on antidepressant drugs for a long time, and many more antidepressants are now accessible, yet binge eating has taken on a new form, determined by the need to reduce weight-study of medications in pharmacotherapy that have direct or indirect effects on appetite has taken place-, for example, fenfluramine, formerly prescribed for weight reduction but no longer available due to heart valve problems.23
The US Food and Drug Administration has authorized the lipase inhibitor orlistat as an anti-obesity drug, the combination of orlistat and CBTgsh led to a substantially greater post-treatment rate of binge eating remission when compared to placebo plus CBTgsh, but not at a 3-month follow-up when both the drug and CBTgsh were stopped.24 and after a lot of trials for several drugs, Several trials used lisdexamfetamine have been the most current attempt at treating BED with medication.25
VR(virtual reality) cue exposure treatment is one of the most widely used contemporary clinical applications in EDs (Eating Disorders )Cue Exposure Therapy (CET). In general, VR-CET reduces anxiety reactions to food-related stimuli and cravings which is a strong and uncontrolled want for a specific meal, which lowers the likelihood of overeating in patients with BN or BED.26 by stimulating the feeling of the patient using VR so he or she will have BED episodes and we will try to control them even using medication or psychological therapy.10
The impact of the COVID-19 pandemic on eating disorders, especially BED:
COVID-19 has a very bad impact on eating disorders as one of the main impacts was feeling lonely. Staying at home caused emotions of loneliness, worry, and melancholy, which exacerbated ED symptoms. According to several types of research, social media and traditional media messages frequently focused on the fear of gaining weight in general; people with EDs found stress and triggers in topics like diet discussion, exercise, and good eating throughout the pandemic.27 However, People who experienced the pandemic reported that lockdown procedures protected them from past stresses or triggers, gave them time to take care of themselves and think, and in some cases, increased their social support.28
Conclusion
Eating disorders affect people of various ages and socioeconomic groups, which have evolved during the past 60 years in the setting of significant environmental changes. These eating disorders take on a range of forms with overlapping and different clinical and etiological characteristics. A meta-analysis of 36 studies mentioned that up to About 26% of people with eating disorders attempt suicide.11 Making EDs potentially lethal. Additionally, they may result in significant health problems as well as significant psychological suffering. As the eating disease consumes time and energy, leads to self-absorption, and lowers self-esteem, important relationships suffer.
Treatment should begin as soon as possible; in order to concentrate on the acute misery the patient is experiencing. Also, work to empower the patient and family to overcome the eating problem.12